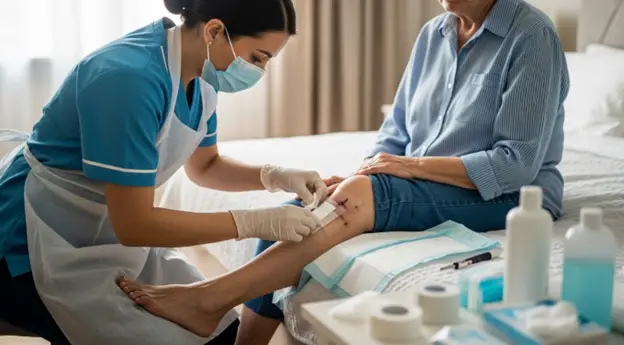
Home healthcare plays a crucial role in helping patients recover comfortably in their own homes. Many families rely on caregivers such as home health aides to assist with daily tasks and medical support. However, when it comes to wound care especially sterile procedures questions often arise about what caregivers are legally and medically allowed to do.
One of the most common concerns families ask is: can a home health aide change a sterile dressing? The answer depends on medical regulations, training requirements, and the type of wound being treated. Understanding these factors is essential to ensure patient safety and proper healing.
This guide explains the responsibilities of home health aides, the medical rules around sterile wound care, and what caregivers can and cannot do in a home healthcare setting.
Short Answer — Can a Home Health Aide Change a Sterile Dressing?
In most situations, a home health aide cannot legally change a sterile dressing. Sterile wound care typically requires a licensed healthcare professional such as a registered nurse (RN) or licensed practical nurse (LPN).
However, there can be limited exceptions depending on several factors, including:
- State healthcare regulations
- Policies of the home health agency
- Direct supervision by a nurse
- The type and severity of the wound
In general, sterile dressing changes involve medical procedures that require advanced training in infection control and wound management. Even though many caregivers complete home health aide certification, this training typically focuses on personal care and basic patient support rather than complex medical procedures. Because of the risk of infection or complications, licensed nurses are usually responsible for performing sterile wound care in home healthcare settings.
Home health aides can still play an important role by assisting with preparation, monitoring the patient, and supporting the nurse during care.
Understanding the Role of a Home Health Aide in Patient Care
What Is a Home Health Aide (HHA)?
A home health aide (HHA) is a trained caregiver who provides non-medical and basic healthcare assistance to individuals receiving care at home. HHAs are commonly employed by home care agencies, hospice programs, and assisted living services.
Most home health aides complete certification programs that include:
- Basic caregiving skills
- Personal care assistance training
- Infection control basics
- Patient safety procedures
While they receive healthcare-related training, HHAs are not licensed medical professionals.
Typical work settings include:
- Private homes
- Assisted living communities
- Hospice care programs
- Home healthcare agencies
Their primary role is to support daily living activities while helping patients maintain independence.
Typical Responsibilities of Home Health Aides
Home health aides assist with a wide range of daily care activities, including:
- Personal hygiene and bathing
- Dressing and grooming
- Mobility and transfer assistance
- Meal preparation and feeding assistance
- Light housekeeping
- Medication reminders (not administering medication)
- Monitoring basic vital signs in some cases
These services are essential for patients recovering from surgery, managing chronic illness, or living with disabilities.
Tasks Home Health Aides Are NOT Usually Allowed to Perform
Despite their valuable role, HHAs are generally restricted from performing clinical procedures that require sterile technique or advanced medical knowledge.
Tasks they are typically not permitted to perform include:
- Sterile medical procedures
- Administering injections
- Managing intravenous (IV) therapy
- Changing sterile wound dressings
- Performing invasive procedures
These duties require professional licensure and advanced clinical training.
Why Sterile Dressing Changes Require Medical Training
What Is a Sterile Dressing?
A sterile dressing is a protective wound covering applied using sterile technique to prevent bacteria or contaminants from entering the wound.
Sterile dressings are commonly used for:
- Surgical incisions
- Deep wounds
- Pressure ulcers
- Severe burns
- Post-operative wound care
Maintaining a sterile environment is essential because these wounds are highly vulnerable to infection.
Risks of Improper Sterile Wound Care
Improper dressing changes can lead to serious medical complications, including:
- Wound infection
- Delayed healing
- Tissue damage
- Cross-contamination
- Sepsis in severe cases
Because of these risks, sterile dressing changes require strict adherence to infection control protocols.
Why Sterile Technique Is Critical in Home Healthcare
Sterile technique prevents harmful microorganisms from contaminating the wound. In home healthcare environments where hospital-level sterilization equipment may not be available proper training becomes even more critical.
Licensed nurses are trained to:
- Maintain a sterile field
- Use sterile gloves and instruments
- Assess wound healing progress
- Identify early signs of infection
These skills ensure that wound care supports recovery rather than causing complications.
Can a Home Health Aide Change a Sterile Dressing Under Supervision?
Situations Where an HHA May Assist With Dressing Changes
Although HHAs typically cannot perform sterile dressing changes themselves, they may assist with certain supportive tasks under nurse supervision.
These may include:
- Preparing wound care supplies
- Positioning the patient comfortably
- Providing emotional reassurance
- Helping maintain cleanliness around the care area
In some cases, HHAs may assist with non-sterile dressing changes, depending on training and agency policy.
State Regulations That Affect Home Health Aide Duties
Healthcare responsibilities vary widely across states. Regulations are often determined by:
- State nursing boards
- Department of health guidelines
- Home health agency policies
Some states allow limited medical tasks if delegated by a nurse, while others strictly prohibit HHAs from performing any sterile procedures.
Because regulations differ, families should always consult their local home healthcare provider or state regulations.
When a Licensed Nurse Must Perform the Dressing Change
A registered nurse or licensed practical nurse is typically required when the wound involves:
- Surgical incisions
- Post-operative recovery care
- Deep tissue wounds
- High-risk infections
- Complex wound management
These cases require professional wound assessment and sterile technique.
Who Is Qualified to Change a Sterile Dressing?
| Healthcare Professional | Allowed to Change Sterile Dressings | Training Level | Typical Care Setting |
| Registered Nurse (RN) | Yes | Advanced clinical training | Hospitals, home health |
| Licensed Practical Nurse (LPN) | Usually yes | Practical nursing training | Clinics, home care |
| Nurse Practitioner | Yes | Advanced practice nurse | Medical practices |
| Home Health Aide | Usually no | Basic caregiving training | Home care |
| Certified Nursing Assistant (CNA) | Usually no | Basic nursing assistance | Long-term care |
Step-by-Step Overview of How Sterile Dressing Changes Are Performed
Step 1: Preparing the Sterile Environment
The healthcare professional begins by:
- Washing hands thoroughly
- Wearing sterile gloves
- Preparing sterile instruments
- Opening a sterile field
This ensures that the wound is protected from bacteria.
Step 2: Removing the Old Dressing Safely
The previous dressing is carefully removed while observing:
- Drainage levels
- Odor or infection signs
- Skin condition around the wound
Used materials are disposed of in appropriate medical waste containers.
Step 3: Cleaning the Wound
The wound is gently cleaned using sterile saline or prescribed cleaning solution. The clinician follows a specific wiping technique to prevent contamination.
Step 4: Applying the New Sterile Dressing
A fresh sterile dressing is placed over the wound while maintaining strict sterile technique to prevent exposure to bacteria.
Step 5: Securing the Dressing and Documenting Care
The dressing is secured with sterile bandages or medical tape. The nurse then records:
- Wound size and appearance
- Drainage levels
- Signs of infection
- Patient comfort and response
Documentation ensures proper monitoring of healing progress.
Sterile vs Non-Sterile Dressing Changes (Key Differences)
| Feature | Sterile Dressing | Non-Sterile Dressing |
| Infection risk | High-risk wounds | Minor wounds |
| Technique required | Strict sterile technique | Clean technique |
| Who performs it | Nurse or clinician | Sometimes aides or caregivers |
| Typical wounds | Surgical wounds, deep ulcers | Minor cuts, abrasions |
| Equipment used | Sterile gloves, sterile field | Clean gloves |
What Home Health Aides Can Do Instead During Wound Care
Supporting the Nurse During Dressing Changes
Home health aides provide valuable assistance by:
- Preparing wound care supplies
- Helping patients sit or lie comfortably
- Offering reassurance during procedures
Monitoring the Patient Between Nurse Visits
HHAs often spend more time with patients than nurses and can observe important changes such as:
- Redness or swelling around the wound
- Increased drainage
- Fever or discomfort
These observations can be reported to the healthcare team.
Helping Maintain Hygiene and Infection Prevention
HHAs help prevent complications by:
- Keeping the wound area clean
- Changing bed linens regularly
- Encouraging proper hygiene
- Reminding patients about care instructions
Signs of Wound Infection Caregivers Should Watch For
Caregivers should notify healthcare professionals immediately if they notice:
- Increased redness
- Warm skin around the wound
- Pus or unusual drainage
- Fever or chills
- Increased pain or swelling
Early detection is critical to prevent serious complications.
Safety Considerations in Home Wound Care
Infection Control in the Home Setting
Maintaining a clean environment is essential for wound healing. Important practices include:
- Frequent hand washing
- Cleaning surfaces before procedures
- Using clean or sterile supplies
- Proper disposal of dressings and gloves
When to Contact a Nurse or Doctor Immediately
Immediate medical attention may be necessary if the patient experiences:
- Sudden swelling
- Severe pain
- Heavy bleeding
- Wound reopening
- Signs of systemic infection
Real-World Home Healthcare Scenario
Consider a patient recovering from surgery who receives care at home. A registered nurse visits several times per week to perform sterile dressing changes and monitor healing.
During the rest of the week, a home health aide assists the patient with bathing, mobility, and household tasks. The aide also observes the wound area and reports any unusual symptoms to the nurse.
This collaborative approach allows the patient to recover safely while receiving continuous support.
Frequently Asked Questions (FAQs)
Can a home health aide change a sterile dressing legally?
In most cases, no. Sterile dressing changes are usually restricted to licensed nurses due to infection risks and required medical training.
Can a CNA change a sterile dressing at home?
Certified nursing assistants typically cannot perform sterile dressing changes unless specifically authorized under strict supervision and regulations.
What is the difference between sterile and clean wound care?
Sterile wound care uses fully sterilized equipment and techniques to prevent contamination, while clean wound care focuses on general cleanliness for minor wounds.
Can family caregivers change sterile dressings?
Family caregivers may sometimes be trained by healthcare professionals to perform dressing changes, but they must follow strict instructions and medical guidance.
How often should sterile dressings be changed?
The frequency depends on the wound type, drainage level, and doctor’s orders. Some dressings are changed daily, while others remain in place for several days.
Who performs wound care in home health services?
Wound care in home healthcare is typically performed by registered nurses, licensed practical nurses, or specialized wound care nurses.
What happens if a sterile dressing is contaminated?
If contamination occurs, the dressing must be replaced immediately to prevent infection.
Do home health aides receive wound care training?
Home health aides receive basic infection-control training but usually do not receive advanced training required for sterile wound care procedures.
Key Takeaways — Can a Home Health Aide Change a Sterile Dressing?
The answer to can a home health aide change a sterile dressing is generally no. Sterile wound care requires advanced training and strict infection control techniques that fall within the scope of licensed healthcare professionals.
Home health aides still play an essential role by assisting patients with daily care, monitoring for complications, and supporting nurses during medical procedures.
When dealing with surgical wounds or complex injuries, always rely on qualified healthcare professionals to perform sterile dressing changes.
Conclusion
Sterile wound care is a specialized medical procedure designed to protect patients from infection and promote proper healing. Because of the risks involved, sterile dressing changes are typically performed by licensed nurses or other trained medical professionals. Healthcare providers, including organizations such as One Health and Beyond, emphasize that proper medical supervision is essential when managing complex wound care to ensure patient safety and successful recovery.
While home health aides cannot usually perform sterile dressing changes, they remain an essential part of the home healthcare team. By assisting with daily care, observing patient conditions, and supporting nurses, they help ensure that patients recover safely and comfortably at home.
For the best outcomes, families should always follow professional medical guidance and ensure that wound care procedures are handled by qualified healthcare providers.