Alt Text: A MAP-certified healthcare worker in Massachusetts carefully verifying a medication label against a MAR to prevent errors.
Medication errors in direct care settings are not rare, and they are not always dramatic. Most of them happen quietly: a missed dose, a wrong time, a pill meant for one resident that ended up in front of another. A single error rarely makes the news, but in group homes, day programs, and community residences across Massachusetts, the cumulative impact is real. Residents miss therapeutic effects, trust with families erodes, and facilities face serious compliance consequences. This guide walks through the medication errors that actually occur in direct care, the protocols MAP training puts in place to prevent them, and why employers across DDS, DMH, DCF, and MassAbility community programs insist on certified staff.
Quick answer: The most common medication errors in direct care settings fall into five categories: wrong resident, wrong medication, wrong dose, wrong time, and wrong route. In Massachusetts, each incident is formally documented as a Medication Occurrence Report (MOR) under DPH regulations. MAP training is built around preventing every category through structured protocols, documentation, and the five rights of medication administration.
Why Medication Errors in Direct Care Matter
Residents in DDS, DMH, DCF, and MassAbility community programs often depend on medication regimens for stability across mental health, seizure control, cardiovascular function, diabetes management, and behavior regulation. An interrupted medication schedule can trigger preventable emergencies within hours. A resident who misses a scheduled antiepileptic dose may experience a breakthrough seizure. A resident who receives another person’s psychotropic medication may face serious adverse effects. A resident who misses blood pressure medication may develop symptoms that require hospitalization.
Beyond the immediate resident safety concerns, medication errors carry documentation and compliance consequences. DPH survey reviews examine medication administration records and Medication Occurrence Reports closely. Employers face citations and sometimes funding consequences when error patterns emerge. Staff responsible for errors face corrective action, retraining, and in severe cases, removal from medication duties altogether.
The Five Most Common Medication Error Categories
Every medication error in direct care falls into one of five categories tied directly to the five rights framework that anchors MAP training. Under DPH regulations, a medication occurrence is defined as a breach of one of these five rights.
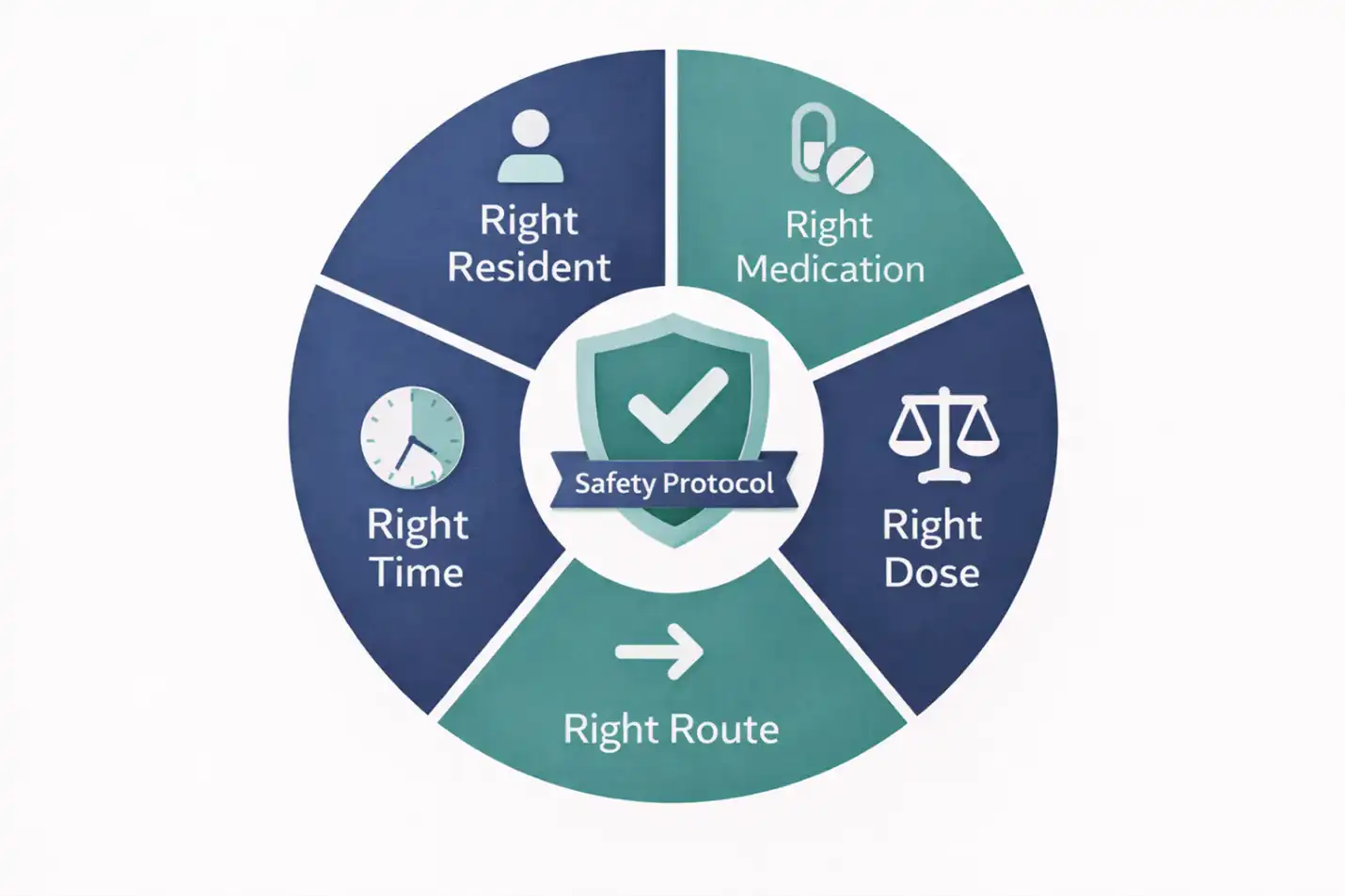
Alt Text: Infographic diagram of the Five Rights of Medication Administration used in MAP training to prevent direct care errors.
1. Wrong Resident Errors
A medication prescribed for one resident is administered to a different resident. This typically happens during busy morning passes when multiple residents are receiving medications simultaneously, or when new staff confuse residents by appearance or room number. Wrong resident errors can be among the most serious because the medication may be contraindicated for the person who actually received it.
2. Wrong Medication Errors
The correct resident receives the wrong medication. Common causes include look-alike pill confusion, sound-alike drug name mix-ups, or failure to verify the medication against the MAR before administration. Medications with similar packaging are a particular risk during fast-paced shifts.
3. Wrong Dose Errors
The right medication is given to the right resident, but in the wrong amount. This includes giving too much, too little, or splitting a pill incorrectly when the order called for a partial dose. Medication math errors frequently live inside this category, which is why MAP training includes extensive dosage calculation practice.
4. Wrong Time Errors
Medications administered outside the prescribed window. For most medications, a one-hour grace period is acceptable under DPH guidelines, but certain medications require precise timing. Antiepileptics, antibiotics, and insulin are examples where timing errors can have immediate therapeutic consequences.
5. Wrong Route Errors
Medication administered through the wrong route, such as giving an oral medication through a feeding tube without proper preparation, or using the wrong application site for a topical medication. Route errors are less common than the other four categories but often cause significant harm when they occur.
MAP Training Protocols That Prevent Each Error Type
MAP training is structured around the specific protocols DPH requires to prevent each category of medication error. Here is how MAP-certified staff address each error type during every medication pass.
| Error Type | MAP Prevention Protocol | Key Verification Point |
| Wrong Resident | Two-identifier verification before administration | Match name and photo ID to MAR |
| Wrong Medication | Three-check rule at pulling, preparing, and administering | Verify against MAR each time |
| Wrong Dose | Medication math verification plus dose double-check | Compare transcribed dose to HCP order |
| Wrong Time | Scheduled pass windows plus documentation timing | Confirm within DPH grace period |
| Wrong Route | Route confirmation at preparation stage | Verify route matches MAR instruction |
The MAP Safety Check: Your Three-Point Daily Routine
MAP-certified staff memorize a three-checkpoint safety routine that runs before every medication reaches a resident’s hand. This checkpoint structure is what the three-check rule looks like in real practice.
THE MAP SAFETY CHECK
Check 1: Pulling From the Lockbox. Verify the label matches the MAR before removing medication from storage.
Check 2: Preparing the Dose. Confirm label, dose, and route match the MAR before pouring or counting the medication.
Check 3: Administering to the Resident. Final verification at the resident, matching name, medication, dose, route, and time.
★ Always match the Label to the MAR — word for word, every time.
The Five Rights Framework as Daily Practice
MAP training teaches the five rights of medication administration not as a classroom concept but as a repeated daily ritual. Before every medication pass, MAP-certified staff verify each of the following.
- Right Resident. Use two identifiers to confirm the resident’s identity, typically name plus photo or room number.
- Right Medication. Compare the medication against the MAR at three checkpoints: when pulling from storage, when preparing the dose, and when administering.
- Right Dose. Verify the dose matches the HCP order as transcribed on the MAR. If partial doses are involved, complete the math calculation and confirm.
- Right Route. Confirm the route of administration, whether oral, topical, inhaled, rectal, or other, matches the MAR instruction exactly.
- Right Time. Administer within the prescribed time window under DPH grace period guidelines, and document the actual administration time.
This five-point check runs before every medication, every time. MAP-certified staff repeat the sequence enough times during training that it becomes automatic during real shifts. That automatic repetition is what turns classroom knowledge into actual error prevention.
Errors MAP Training Also Prevents
Beyond the five rights framework, MAP training addresses several other error categories that occur in direct care settings.
✓ Documentation Errors. Incomplete or late MAR entries cause confusion during shift changes and may lead to duplicate doses or missed doses. MAP training teaches exactly when and how to document administration.
✓ Transcription Errors. Incorrect transcription of an HCP order onto the MAR is a root cause of many medication errors. MAP training includes a dedicated transcription component, and the D&S certification test evaluates this skill separately.
✓ PRN Judgment Errors. PRN medications require judgment about when administration is appropriate. MAP training defines the boundaries of PRN decision-making and the documentation that must accompany every PRN pass.
✓ Storage and Counting Errors. Medications must be stored securely with accurate count tracking for countable medications. MAP training covers double-lock requirements, count procedures, and disposal protocols.
✓ Refusal Documentation Errors. When a resident refuses a medication, staff must document the refusal correctly and notify the appropriate supervisor. Incomplete refusal documentation can lead to compliance issues during DPH review.
What MAP Staff Do When an Error Happens: The MOR Process
Despite training and structured protocols, medication errors still occur in direct care settings. When they do, Massachusetts requires a formal Medication Occurrence Report (MOR) under DPH regulations. Hiding an error is a more serious violation than making one, and failing to file an MOR within the required timeframe can result in facility citations and corrective action for individual staff.
The Massachusetts MOR process prioritizes resident safety first, then accurate documentation and reporting. MAP-certified staff follow a specific response protocol when an error occurs.
- Assess the Resident First. Check for any immediate adverse reaction, signs of harm, or urgent medical needs.
- Notify the Supervising Nurse. Contact the supervising nurse or on-call medical authority immediately after ensuring resident safety.
- Complete the MOR Form. Document the incident on the DPH Medication Occurrence Report (MOR) form with accurate details including what was administered, what should have been administered, the time, and any observations.
- Submit Within DPH Timeframes. Non-hotline MORs must be submitted to the appropriate DMH, DCF, DDS, or MassAbility MAP Coordinator within seven days. Hotline MORs, which involve medical intervention, illness, injury, or death, must be submitted to DPH within 24 hours.
For DDS-operated sites, MORs are filed through the Home and Community Services Information System (HCSIS). Staff who respond to errors correctly demonstrate competency even when something went wrong. Staff who hide errors or falsify documentation face serious corrective action and may lose MAP certification entirely.
Why Employers Insist on MAP-Certified Staff
Employers who operate DDS, DMH, DCF, and MassAbility community programs rely on MAP-certified staff for three clear reasons. The certification signals that staff have completed structured DPH-approved training in error prevention. The D&S testing process verifies competency on knowledge, transcription, and live medication administration. The worksite practicum confirms that the staff member can perform medication passes correctly under real conditions.
Non-certified staff simply cannot offer that assurance. Agencies, group home operators, and day program directors face serious liability and compliance risks when non-certified staff perform medication administration, which is why open MAP positions across Massachusetts consistently pay a premium over equivalent non-MAP roles.
→ Ready to be the most trusted staff in the facility? Enroll in our next MAP Class in Stoughton and walk into your next shift with the credential employers trust.
Become the Staff Employers Trust Most
MAP certification is the credential that demonstrates you can prevent medication errors under real pressure and document every incident correctly when something does go wrong. Our Stoughton campus runs DPH-aligned MAP classes on flexible evening and weekend schedules. Reserve your seat in the next MAP class today.
Still confirming eligibility? Review our MAP certification requirements guide. Curious about what the class looks like? See what happens in a MAP class. Comparing paths? Read MAP vs LPN: Can You Administer Medications Without Being a Nurse?.







